In the Bethesda System (TBS) for cervical liquid-based cytology, High-Grade Squamous Intraepithelial Lesion (HSIL) represents a critical diagnostic threshold. It indicates that a cervical lesion has progressed to a stage requiring high clinical vigilance and proactive intervention. Accurate interpretation directly impacts the timeliness and precision of subsequent clinical decision-making. Today, we will systematically review the diagnostic essentials of HSIL.
1. Cell Size:
HSIL cells are generally smaller than LSIL cells and exhibit lower cytoplasmic maturity.
While cell size may vary, HSIL cells are overall smaller than those of LSIL. High-grade lesions often contain a significant population of small, parabasal-type cells.
2. Nucleus:
Nuclear Enlargement: Inconsistent compared to LSIL. Some HSIL cells show nuclear enlargement similar to LSIL but with significantly increased Nuclear-to-Cytoplasmic (N/C) ratios due to decreased cytoplasm. Others have very high N/C ratios but smaller absolute nuclear size (sometimes as small as a normal intermediate cell nucleus).
N/C Ratio: Consistently higher in HSIL than in LSIL.
Hyperchromasia: Nuclei are typically hyperchromatic but can be normochromatic or even pale.
Chromatin: May be fine or coarsely granular, but is uniformly distributed.
Nuclear Membrane: Distinctly irregular contours, often with prominent indentations or notches.
Nucleoli: Generally absent, though occasionally observed, particularly when HSIL involves endocervical gland spaces or occurs in a background of reactive/reparative changes.
3. Cytoplasm:
Displays varied morphology; may appear "immature," delicate/lace-like, or present as dense metaplastic staining. Occasionally, cytoplasm may appear "mature" with dense keratinization (Keratinizing HSIL).
4. Cellular Arrangement:
Cells may occur singly, but typically present in "crowded sheets" or "syncytial-like" aggregates with indistinct cell borders.
Mnemonic: Large hyperchromatic nuclei, high N/C ratio, pleomorphic shapes, and disordered arrangement.
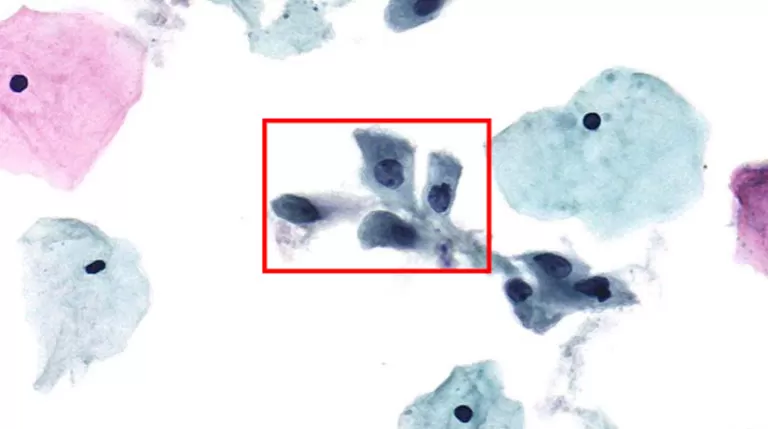
Figure 1: Typical HSIL Morphology Note: Prepared via HealthSky SCTE-3600A SCT Method; Reviewed with HealthSky Patho. AI-Assisted Diagnostic System.
1. HSIL in Atrophic Background:
Challenge: Atrophic epithelial cells are often small with nuclear crowding and high N/C ratios, which may lead to overdiagnosis.
Key Differentiation: HSIL cells exhibit more pronounced nuclear abnormalities (coarser chromatin, more irregular membranes) and create a "discordant" appearance against the atrophic background. Follow-up after estrogen therapy can aid differentiation.
2. HSIL Involving Endocervical Glands:
Challenge: Easily misidentified as glandular lesions or Adenocarcinoma In Situ (AIS).
Key Differentiation: HSIL clusters typically have smooth borders with a "whorled" center, retaining squamous characteristics and disordered nuclear polarity. In contrast, AIS clusters are more organized, exhibiting "feathering," "rosettes," and pseudostratified palisading columnar cells.
3. HSIL with Inflammatory or Reparative Changes:
Challenge: Severe inflammation or repair can cause cellular/nuclear enlargement and prominent nucleoli, mimicking neoplasia.
Key Differentiation: Reparative cells usually have smooth nuclear membranes, fine granular chromatin, and maintained polarity. Irregular nuclear membranes and coarse/clumpy chromatin are hallmarks of HSIL. While nucleoli are rare in typical HSIL, their presence should raise suspicion of potential invasion.
Features | High-Grade Squamous Intraepithelial Lesion (HSIL) | Squamous Cell Carcinoma (SCC) |
Cell Morphology | Relatively consistent; despite atypia, an "epithelioid" structure is maintained. | Marked pleomorphism; bizarre-shaped cells (e.g., spindle cells, tadpole cells) may be present. |
Nuclear Features | Nuclei are large and hyperchromatic, but size remains within a certain predictable range. | Extreme nuclear atypia: extreme variation in size, bizarre shapes, and chromatin appearing as coal-clumps or "ink-drops." |
Nucleoli | Typically inconspicuous or absent. | Large, prominent, multiple, and irregular nucleoli are critical warning signs. |
Background | Usually clean, or may be accompanied by inflammation. | Typical tumor diathesis: necrotic debris (dirty necrotic background), old hemorrhage, and inflammatory cell infiltration. |
Cellular Arrangement | Crowded sheets or syncytial-like aggregates. | Predominantly isolated and scattered distribution, indicating a loss of intercellular cohesion. |
Core Reminder: If you observe prominent nucleoli, extreme pleomorphism, or a diathesis (tumor necrosis) in an HSIL field, the possibility of Squamous Cell Carcinoma (SCC) must be considered immediately and noted in the report.
Clinical management for women with HSIL includes: Colposcopy with cervical biopsy and Endocervical Curettage (ECC) to detect high-grade lesions. Subsequent treatment depends on biopsy results.
Patients ≥ 25 years: If HSIL is cytologically confirmed and a lesion is identified during colposcopy, immediate excision is recommended.
Biopsy-unconfirmed HSIL: If colposcopy fails to identify a lesion after an HSIL cytology result, a thorough review of cytological and histological specimens is required. Additional sectioning and p16 IHC staining may be utilized to reveal occult lesions.
Special Populations (Pregnancy): Colposcopy by an experienced clinician is recommended; however, ECC is unacceptable. If no histological HSIL is found, a follow-up is recommended six weeks postpartum.
Accurate HSIL interpretation is a pivotal link in cervical cancer screening. It requires pathologists to maintain a "keen eye" to capture essential features amidst complex morphologies, distinguish mimics, and remain alert for invasion.
HealthSky is committed to providing premium LBC liquid-based cytology products and services, partnering with you to safeguard women’s cervical health.